Why Your Child Always Seems Sicker at Night: A Pediatrician Explains
Why evenings feel harder, what’s happening in your child’s body, and how to respond with confidence
It’s 9:07 pm.
Everyone is finally in their pajamas, your washing machine is working overtime…and suddenly the cough starts. Or the fever spikes. Or your kid has an epic meltdown worthy of an Academy Award (they are extraordinary after all!).
If you’ve ever thought, “Why does everything ALWAYS get worse at night?”, you are not imagining it! Plenty of parents across the centuries have whispered the exact same question…usually while pacing a dark hallway.
And of course, it happens right when your pediatrician’s office is closed, your mom is already in bed, and you’re just hoping for five minutes of peace before you turn out the lights.
But there are real physiologic reasons this happens. In this post, I will break down the science behind the nighttime chaos, share practical tips for easing nighttime symptoms, and help you recognize when something needs more attention.
Let’s do it!
Gravity: The Great Mucus Mover
If you’ve ever stepped foot into a daycare, you know kids are really snotty. Like REALLY snotty. All those sweet, adorable babies…with a constant stream of mucus. Seriously, is there a commercial operation going on inside those little noses? A high-efficiency factory churning out snot 24/7?
And we all know the factory does not turn the lights off once 5 pm hits. Nope, we aren’t that lucky!
So imagine your sweet little kiddo lays down at night. And all that snot that was running out of the front of their nose while they were upright, is now running down the back of their nose instead (thanks, gravity). It pools in the back of their throat and lingers.
Our bodies are always behind the scenes trying to keep us healthy and safe. Cilia, tiny hairlike structures that line the airways, serve as miniature mucus movers. But lying flat makes that job harder. More post-nasal drip occurs, the cilia can’t channel their inner Elphaba and defy gravity, and the mucus pools in the back of the throat. This activates the cough receptors, and the coughing revs us.
Just when you are settling into bed.
The result? Congestion becomes more obvious at night, coughing increases, and suddenly everyone is…just a bit more miserable.
💡Fun Fact: Kids produce more mucus than adults because their immune systems are still developing and responding vigorously to new germs. So more “first-time exposures” means more mucus. Fun indeed.
Circadian Rhythms: Your Body’s Internal Clock at Work
If you’ve ever noticed that your child wakes up at the same time every day (even on Saturdays!), or seems to melt down right around dinner time, you’ve witnessed circadian rhythms in action.
Circadian rhythms are the body’s 24-hour internal cycles that regulate everything from sleep to hormones to body temperature. Think of them as the body’s master schedule.
And the conductor of this internal orchestra? A tiny structure in the brain called the suprachiasmatic nucleus (SCN).
The SCN sits deep in the hypothalamus and acts like the body’s timekeeper. It uses light and dark cues to tell the rest of the body when to wake, sleep, release hormones, and even adjust temperature.
Pretty impressive for something smaller than a grain of rice, right?!
So How Does This Affect Nighttime Symptoms?
Circadian rhythms are behind a lot of symptoms that worsen at night in sick kids.
Circadian Rhythms Lower Cortisol at Night
Cortisol is a hormone that is produced by the body to help it function normally. It is produced by the adrenal glands, which are little triangle-shaped organs that sit on top of each kidney. The pituitary gland in the brain tells the adrenals when to release cortisol.
Cortisol is vital for many things in the body:
Managing the body’s stress reaction
Fighting infection
Regulating blood sugar
Maintaining blood pressure
Helping the body use energy
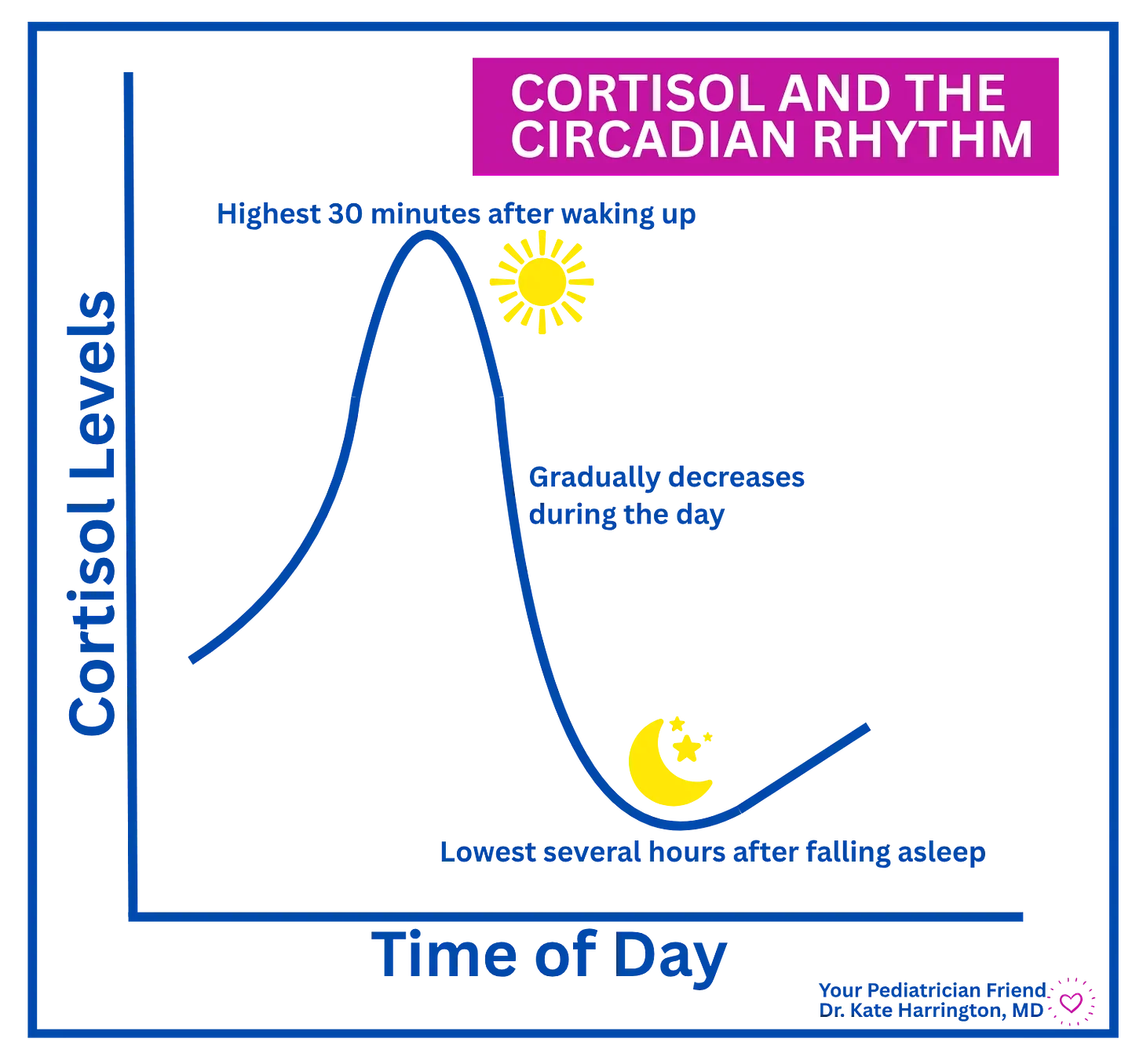
Cortisol follows a circadian rhythm:
Highest levels are present about 30 minutes after waking up
Levels gradually decrease throughout the day.
Lowest levels occur in the middle of the night, several hours after falling asleep
So just imagine: You put your sick kid to bed at 7 pm. At 10 pm, you are exhausted and settling in for a nice night’s sleep. But, that is exactly when your child’s cortisol levels have reached their lowest point. And symptoms flare. Ugh!
When cortisol drops, inflammation naturally increases. Kids who are already fighting a virus have more inflammatory signaling, so they’re primed to feel worse overnight. Inflammatory cells activate the immune system to increase production of interleukin-13 and histamine, prompting the body to make more mucus.
Body Temperature Naturally Rises at Night
Body temperature also follows a circadian rhythm. It reaches its lowest point just before waking in the morning and its highest point in the evening, independent of illness.
For sick kids, this normal temperature rise in the evening coupled with increased cytokine production by the immune system in response to inflammation (thanks, cortisol), leads to a fever spike.
Symptoms Flare with Increased Inflammation and Higher Temperatures
Because of circadian rhythms, we see more mucus, more coughing, more discomfort, more fever, and more”Mom, can you come here?” moments at night.
None of this means that your child is getting dramatically sicker. It just means that their body is working exactly as it is supposed to. Obviously, we parents were not consulted during the design process!
🩺 Pediatrician's Insight: Nighttime fevers spikes are expected. What matters most is how your child looks, acts, and responds once the fever decreases or a fever-reducer is given.
Pain and Emotions Intensify When Kids Are Tired
A tired kid has a much lower capacity to cope with discomfort. Fatigue magnifies everything—emotions, pain, anxiety and frustration. And we all know this to be true: a kid who shrugged off a mild cough at 4 pm suddenly feels miserable at 9 pm.
Low light at bedtime can also heighten anxiety. We all are familiar with kids’ big imaginations going into hyperdrive when they are alone in the dark…the monsters (who were not present all day) are under the bed!
Finally, quiet magnifies sensations that your child may not have even noticed while they were busy all day long. What’s happening with your body becomes a nice thing to focus on while you are laying in bed with no other distractions.
So, nighttime is not only harder physically, it’s also more difficult emotionally. Double whammy!
💡Fun Fact: Pain sensitivity is also affected by circadian rhythms. General pain sensitivity peaks at night (although it varies based on the cause of pain), and lower levels of anti-inflammatory hormones at night (like cortisol) also contribute to discomfort.
Why Nighttime Coughs Sound So Dramatic
We’ve learned that decreased cortisol production at night leads to increased inflammation. As a result, mucus production ramps up, and because of gravity, it pools in the back of the throat. Cough receptors are activated and increased coughing ensues. But, another big contributing factor is dry indoor air.
Heating systems in the winter pull moisture out of the air, making bedroom air drier. Dry air further irritates those cough receptors in the airways and makes nighttime coughing more dramatic.
Finally, remember cilia, those miniature mucus movers in the airways? Dry air makes them a bit slower and less effective at moving mucus out of the airways.
So, dry air + sluggish cilia + more mucus + lying flat = MEGA COUGHING FITS
🩺 Pediatrician's Insight: A cool-mist humidifier, nasal saline spray, and some steamy air from a shower or bath before bed can all help soothe dry airways and move mucus along. But how can you get your child to try nasal saline? Try to have your child give their favorite stuffed animal nasal spray first, then let the stuffie spray your child. Make it as fun as possible!
What Parents Can Actually Do at Night
Although it seems like the odds are against us, there are things that parents can do at night to make things a bit more tolerable for everyone.
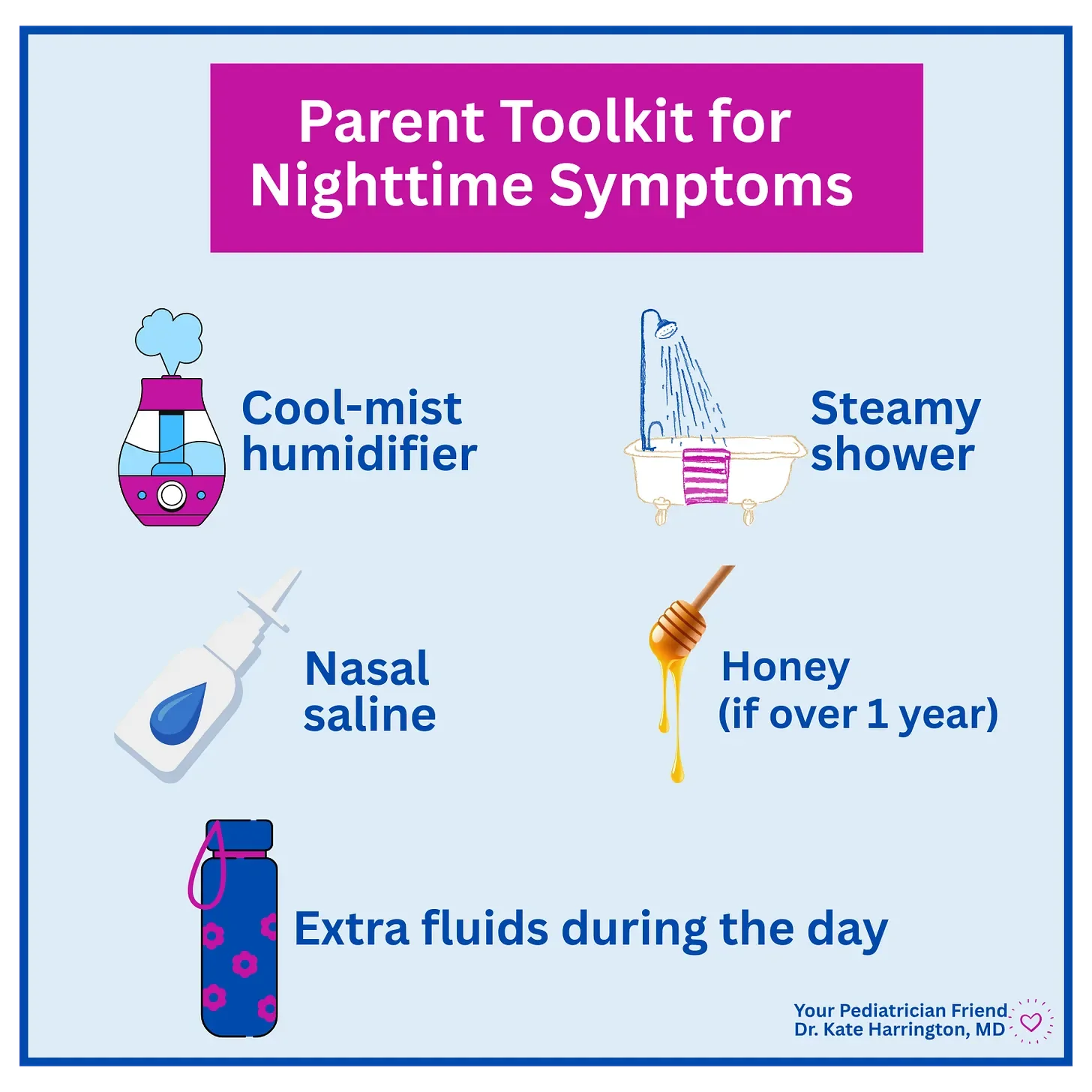
Here are simple, effective tools that help:
Cool-mist humidifier
Nasal saline (hypertonic nasal saline may slightly shorten viral symptom duration and decrease contagiousness)
Nasal suction for babies and toddlers
Steamy air from a warm shower before bed
Honey for kids over 1 year
Hydration during the day (much more effective than overnight drinking)
Don’t wake children to check temperatures or give fever-reducers
Use fever-reducers when a child feels miserable, not based on just the number on the thermometer
You don’t need an entire pharmacy to be prepared for a sick kid at night. Small, simple interventions are usually what helps the most.
🩺 Pediatrician's Insight: When you've got a sick kid, make a “nighttime plan” early in the evening: what remedies you’ll try first, and when you will call the pediatrician or head to the ER. It is easy to feel overwhelmed and unsure at 3 am when things are falling apart! This will help you feel confident and prepared.
When You Should Worry
Call your pediatrician or seek care for:
Trouble breathing (rapid breathing, retractions, flaring)
Signs of dehydration (less than one wet diaper/pee in 8 hours, dry mouth, no tears)
Fever of 100.4°F or higher in a baby under 2 months
Severe lethargy or “not acting right”
Persistent high fever paired with poor appearance
Always trust your gut—you know when something is off 💕
The Bottom Line
Kids’ symptoms often seem worse at night because of gravity, circadian rhythms causing natural drops of cortisol and rises in temperature, dry air, and good old-fashioned fatigue. Understanding these patterns helps you respond with more confidence, less panic, and less fear.
And if nighttime symptoms ever leave you second-guessing what to do, I launched 15-minute virtual consults this week to help you navigate the difficult moments.
You’ve got this! And, you don’t have to figure it out alone 💕