Understanding Your Child’s Cough
A pediatrician’s inside scoop: when to worry, when to wait, and what’s really happening in those tiny airways.
That Endless Cough…
Your child won’t stop coughing, and you feel that anxiety swell in your chest. Should you bring them in, or just wait it out? How do you know if it’s something more serious?
Well, you are not alone if you worry about your child’s cough. And it’s hard not to—it’s a frequent reminder pinging in your ear that something is not quite right. Cough is one of the most common reasons kids see a doctor in the U.S. And pediatricians see kids with coughs (wet coughs, dry coughs, barky coughs, all types of coughs!) many times a day, every single day.
But, how do pediatricians actually think through coughing? When do we worry, and when do we simply watch and wait? Let’s break it down!
What Is a Cough?
Simply put, a cough is a reflex that keeps the airways clear. It’s part of your body’s built-in defense system, triggered by a complex reflex arc that detects irritants like dust, smoke, allergens, germs, mucus, and even a tiny Lego piece that accidentally finds its way into your toddler’s mouth.
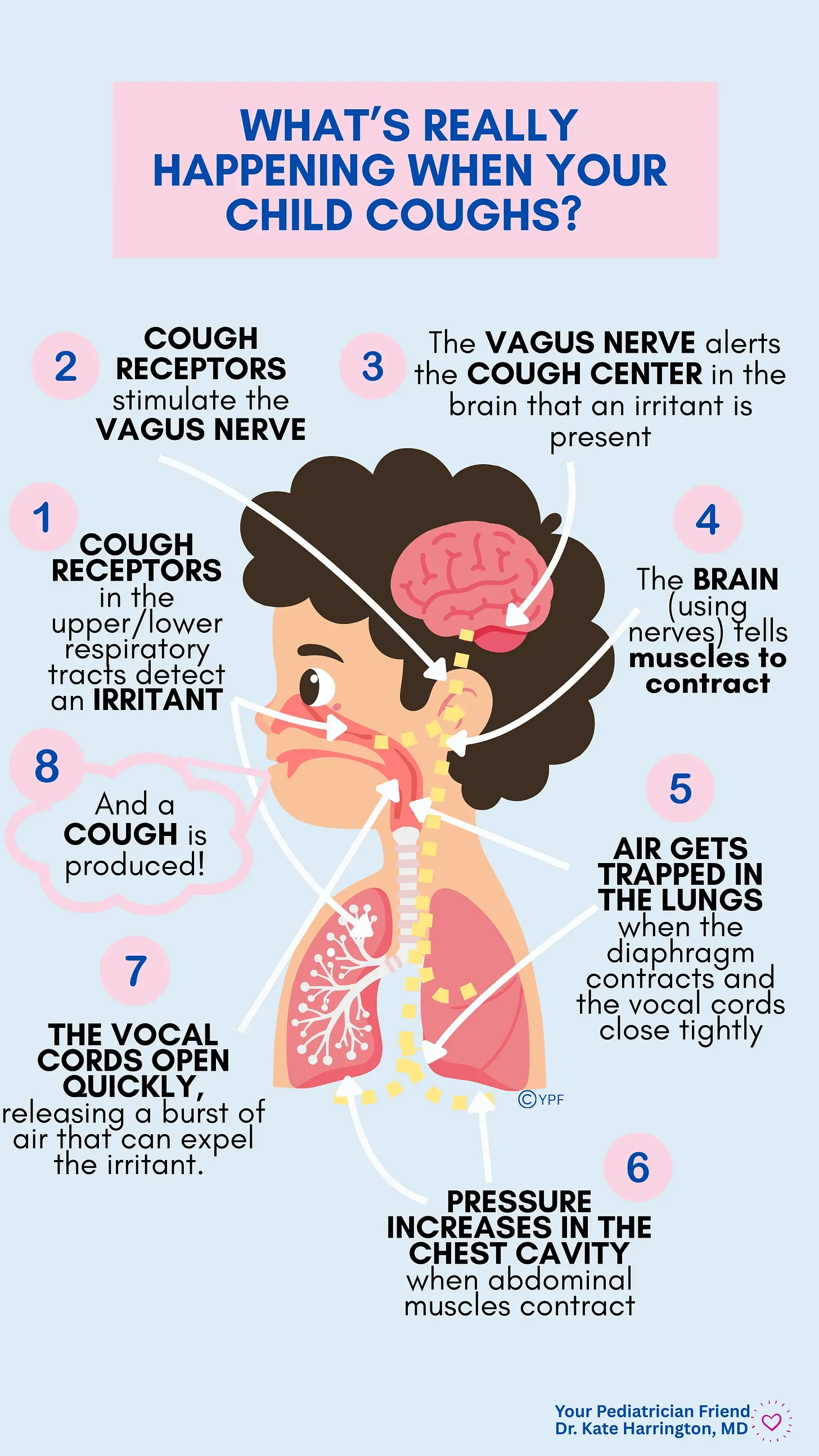
What Happens in the Body When We Cough?
We actually have cough receptors scattered throughout our bodies (not just the lungs!). You’ll find them in the ears, throat, airways, esophagus, and even the stomach.
When these receptors detect an irritant, they activate the vagus nerve. The vagus nerve is a very important part of our parasympathetic nervous system (often called the rest and digest system), and is responsible for the regulation of many different body systems including breathing, digestion, heart rate and the immune system. It starts in the brainstem, runs through the neck and chest, and ends in the abdomen.
Once the vagus nerve is activated by the cough receptors, it notifies the brain’s cough center in the brainstem (called the medulla oblongata…fun to say, right?). From there, signals are sent back through the vagus nerve, spinal motor neurons, and phrenic nerve to coordinate muscle contractions in three stages:
Inspiratory phase: The diaphragm contracts, drawing air into the lungs while the vocal cords close tightly, trapping air inside the lungs.
Compressive phase: Abdominal muscles forcefully contract to increase pressure in the chest cavity,
Expiratory phase: The vocal cords open rapidly, releasing a burst of air—and the irritant is expelled!
➞Voilà : a cough!
Anatomy 101: Where Coughs Come From
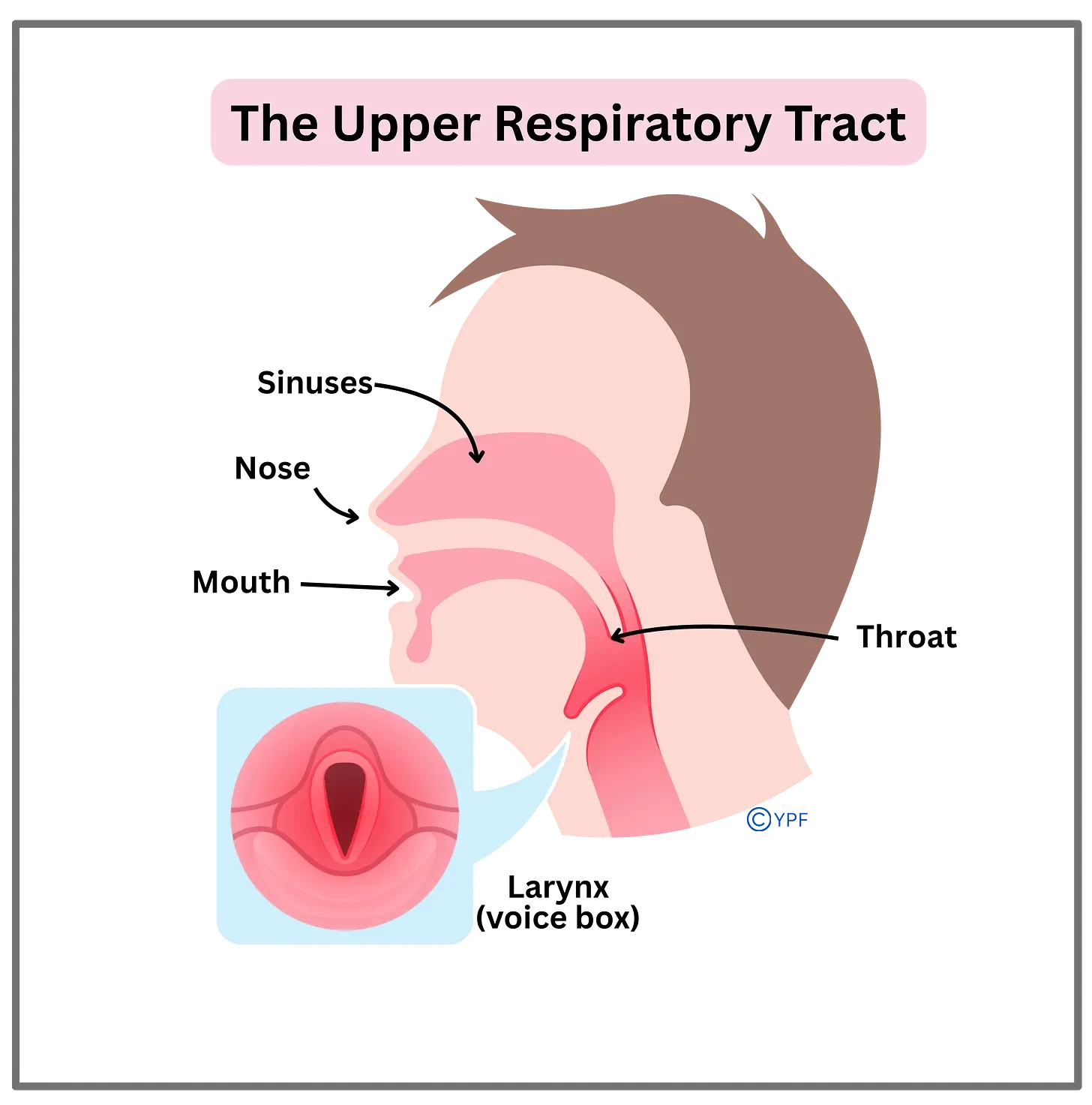
Upper respiratory tract: The upper respiratory tract consists of all those structures above the trachea or windpipe: the nose, mouth, sinuses, throat and larynx (voice box).
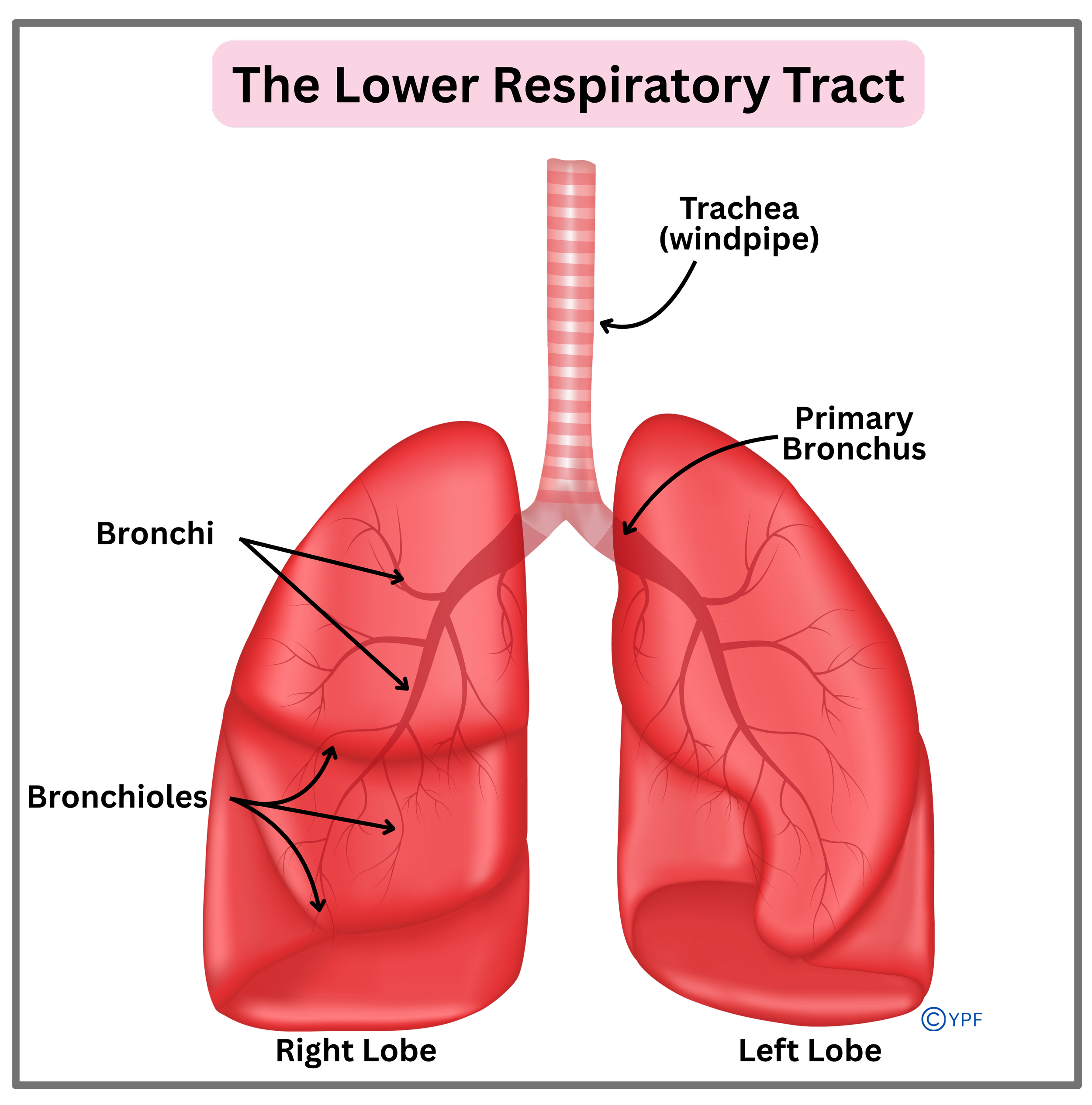
Lower respiratory tract: The lower respiratory system consists of the windpipe (trachea), bronchi (two main branches after the trachea splits), bronchioles (smaller branches of the bronchi), and alveoli (tiny air sacs at the end of the bronchioles where gas exchange occurs between the lungs and blood).
💡Fun Fact: Did you know that you have cough receptors in your ear canals too? Some people cough every time their ears are examined at the doctor. And, an ear problem can even cause a chronic cough—”wild, right?
What’s Normal for a Cough
How long coughs usually last
Most coughs from viral infections will improve by two weeks, and are gone by four weeks. Doctors only call it a chronic cough in kids if it lasts longer than four weeks (eight in adults—sorry parents!).
This feels like a long time! But, as long as the cough is getting better at the two week mark and they feel okay otherwise, you can usually keep monitoring at home.
How coughs sound
There are many normal sounds for cough. They can be dry or juicy, short or hacking, and come in fits.
Certain “flavors” of cough can give pediatricians clues:
Barky cough: often croup
Whooping sound: can be pertussis (whooping cough)
Wet cough: mucus in lower airways (bronchitis, bronchiolitis, pneumonia)
Dry cough: irritation, allergies, or asthma
🩺 Pediatrician’s Insight: Sometimes at the end of an illness, a cough can get a bit worse and sound more junky before it gets better. But, this is often the body’s immune system sending out more mucus to round up the last of the virus. As long as they are otherwise acting normally, you can monitor it for a few days!
Why nighttimes are often worse
You are finally lying down after a busy day, and all you can hear is your child coughing. Ugh! But, remember that this is a very common thing. As kids lay down, mucus pools in the back of the nose and throat, triggering cough receptors to do their job! As long as your child can sleep and isn’t working hard to breathe, it’s okay!
When to See the Doctor for a Cough
Breathing Problems
The most important reason to see a doctor with a cough is if your child has trouble breathing. Watch and listen for these signs:
Fast breathing (more than 60 breaths per minute in infants, or noticeably faster than usual)
Using extra muscles to breathe (nostrils flaring, chest pulling in between ribs, neck muscles tightening)
Noisy breathing (wheezing, stridor)
Very tired or struggling to stay awake
Lasting longer than 4 weeks
Most coughs in children will start to get better by the two week mark of the illness, and go away by four weeks. If a cough lingers beyond four weeks, your pediatrician will want to look for causes like asthma, allergies, sinus infection, pertussis, or lingering infection.
Associated fever
Fevers are normal at the start of many viral illnesses and usually only last a few days. Call your doctor if:
Fever is over 105°F
Fevers lasts more than 5 days
Fever goes away for 24+ hours, but then comes back
These patterns suggest a bacterial infection, and your child may need antibiotics.
Coughing up blood (hemoptysis)
Scant streaks of blood in mucus after hard coughing are common and not dangerous. But, if there is true hemoptysis (more than streaking—which is very rare in kids!), your pediatrician will investigate. Most often it is caused by an infection (like tuberculosis or bacterial pneumonia), but rarely may indicate something more serious.
Persistent cough after a choking episode
If your child choked recently (even a week or two ago), and now has a persistent cough, see your pediatrician. Occasionally a tiny piece remains lodged and keeps irritating the airway.
🩺Pediatrician's Insight: When parents bring their child in for a cough, one of the first things I do is just watch them breathe before I even touch a stethoscope. How a child looks tells me more than any test.
Preparing for a Doctor’s Visit for Cough
Be prepared to answer your pediatrician’s favorite questions about cough:
How long has your child been coughing?
Is your child’s cough accompanied by any other symptoms? And when did those associated symptoms start?
Any trouble breathing?
What does the cough sound like?
Is the cough getting better, worse or the same?
Is the cough interfering with sleep or activity?
Has this happened before?
Anyone else at home coughing?
What have you tried so far?
🩺Pediatrician's Insight: If your child's cough has been associated with a funny sound or breathing issue, take a video and bring it along! We all know how symptoms magically disappear in the clinic!
When an X-ray May Be Needed for Cough
Most children with cough will not need an x-ray, especially if it is associated with a cold or mild pneumonia. However, your pediatrician may consider an x-ray if your child:
Has been coughing more than 4 weeks
Coughs up blood
Had a choking episode
Has signs of bacterial pneumonia (fever, abnormal breathing), but a normal chest exam
Has chest pain or breathing problems that don’t match the physical findings
Managing Coughs at Home
Okay, so you have concluded that your child has just a normal, run-of-the-mill viral cough. And since they have no red flags, like breathing issues or prolonged, high fevers, you decide to stay home. Yay! But now what?
Fluids
Fluids are the mainstay of treatment for a child with a cough. Fluids thin mucus and help the body clear it out. They also help manage fever and keep energy up.
Humidity
Use a cool-mist humidifier by the bed, or try a steamy shower or bath. Nasal saline sprays also help moisten airways and make mucus easier to clear.
💡Fun Fact: Hypertonic nasal saline spray has been shown to decrease the duration of a cold AND decrease contagiousness. Now if your child will just let you do it!
Honey (for kids over 1 year)
Honey soothes the throat and calms those cough receptors. You can just give them a teaspoon straight, or mix it in some warm water or tea.
Cough medicine
Cough suppressants don’t work well in kids under age 6. And remember: cough isn’t always the enemy—it’s a sign the body is doing its job.
However, if you have a child over the age of 6, and their cough is keeping them from sleeping despite extra fluids, humidity, and honey, an occasional bedtime dose of cough medicine can help. I like Delsym (dextromethorphan), a 12 hour cough suppressant, for this purpose (and only for this purpose!!).
Prevention
And of course, the best way to prevent many coughs is regular handwashing, staying up to date on vaccines, and teaching kids to cover their coughs with their elbows!
The Takeaway: Cough Isn’t Always the Enemy
Coughs can be anxiety-provoking. But most coughs are just your child’s body doing exactly what it is supposed to do: protecting the airways and fighting infection.
Keep calm, keep them comfortable, and know when to check in.
Hang in there! You’ve got this 💕