Fever Phobia: Why Fever Isn't the Enemy
Fevers are rarely dangerous...but they feel that way!
So, What’s the Deal with Fevers?
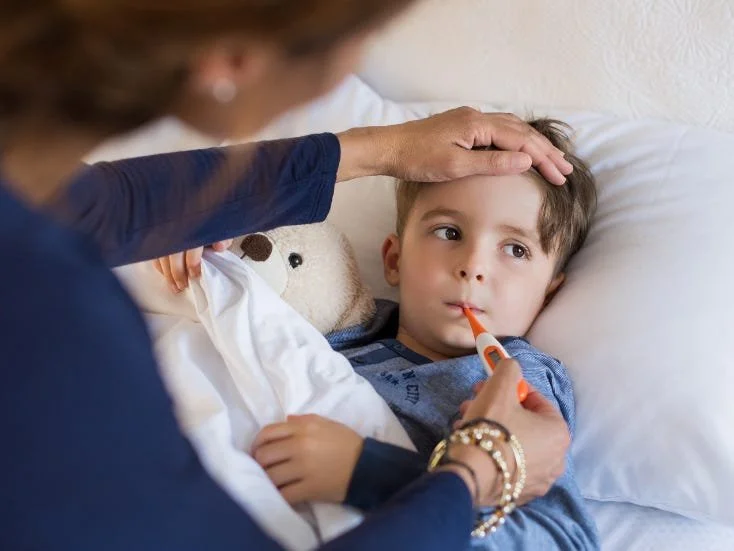
Few things strike fear in a parent’s heart quite like seeing 102°F flash on the thermometer…suddenly you are googling “when can a fever cause brain damage,”texting your pediatrician friend (hey—that’s me! 👋), and wondering if you should start packing your bags for the hospital.
Take a deep breath! Fever isn’t the enemy—it’s a signal that your child’s body and immune system are doing their job!
But there is no question that a fever feels scary. And there is so much contradictory advice out there: sweat it out, never treat it, start medication immediately. Ugh!! What should you do?
I’m here to help! In this post we’ll talk about what actually counts as a fever, how the body regulates temperature, why kids often run hotter than adults, how to treat a fever, and when it’s time to worry. And spoiler alert: it is not as often as you think!
What Is a Fever, Really?
Let’s take a closer look at what’s actually happening inside your child’s body when they spike a fever. In simplest terms, a fever is an abnormal elevation in body temperature. It is a biologic response, and a sign that your child’s immune system is fighting off an infection. While it is controlled by the brain, the process involves many different body systems working together in an impressively coordinated way. (Go body!)
And defining fever and normal body temperature is not quite as straightforward as you think—body temperature varies with age, time of day, activity level, and even hormones (hello periods and perimenopause—I’m talking about you!).
So, let’s start with the basics. What’s a normal temperature, and why does it matter?
What Is a Normal Body Temperature?
The average normal temperature is generally considered to be 98.6°F (37°C). But there are lots of factors that can cause some variation, so that number is more of an average than a universal truth. Everyone runs a little differently, and babies and young children generally have higher normal temperatures than older kids and adults.
Why? Because babies and young children have higher metabolic rates and they have a greater surface area-to-body weight-ratio. Translation: they have more skin exposed to the environment per pound of weight as compared to adults. So, they are more likely to gain heat (or lose it) as compared to someone older.
Here’s a general idea of what’s normal by age and method of measurement:
Newborns: average rectal temperature of 99.5°F (37.5°C), with an upper limit of 100.3°F (38°C)
Older children and adults: average normal temperature of 98.6°F (37°C), with an upper limit of 99.9°F (37.7°C)
And different sites of the body have their own normal ranges of temperatures:
Rectal temperatures are considered to be most reflective of true core body temperature.
Ear temperatures are thought to be roughly equivalent to rectal temperatures.
Oral, underarm, and forehead temperatures are thought to be lower than the rectal temperature, and can be more variable from one reading to the next.
And just to keep things interesting, normal temperature fluctuates throughout the day. Temperatures are lowest in the morning, and peak in the late afternoon/early evening (you read that right—just in time for your pediatrician’s office to close).
So, What Number Actually Counts as a Fever?
The answer depends on where you are sticking that thermometer!
Rectal: 100.4°F or higher
Oral: 100.4°F or higher
Underarm (axillary): 99°F or higher
Ear: 100.4°F or higher
And although normal body temperatures can vary by age, a fever is a fever no matter your age. Whether we get nervous about it depends on how your child looks and age. Spoiler alert: newborns are a special case—more on that later!
How to Check Your Child’s Temperature?
There are plenty of places to check a temperature: rectum, mouth, underarm (also called the axilla), ear, or forehead. And the best method to use is the one that your child (and you!) can tolerate.
Let’s talk about our options:
Rectal (most accurate): This is the reference standard for measuring core body temperature, and is the best way to check a temperature in a baby under 3 months. Taking a rectal temperature can be daunting, especially the first time. But, it is easier than you think, and it will be okay!
Be sure you have a rectal thermometer with a flexible tip.
Clean your thermometer and lubricate the tip with some Vaseline or Aquaphor.
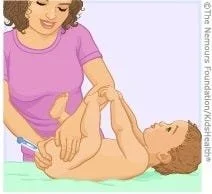
Place your child on their back like you are going to change their diaper, and bend their legs toward their chest. Keep your child steady with your hand against the back of their thighs, while you hold the thermometer in the opposite hand.
Gently insert the thermometer (it will have a guide to tell you how far—don’t force it, and stop if you feel any resistance) and hold it in place until it beeps.
You did it! A newborn is considered to have a fever if their rectal temperature is 100.4°F (38°C) or above.
Oral: This is the method that is generally preferred once a child is old enough to cooperate.
Place the thermometer under your child’s tongue and hold it in place until it beeps.
Because of mouth breathing (one of the ways our body cools itself down with a fever), an oral temperature will generally be about 1°F (0.6°C) LOWER than a rectal temperature.
Oral temperatures can also be affected by drinking hot or cold liquids (did anyone else try to use this to their advantage as a kid?!?).
Axillary: This method is quick and easy, but less accurate.
Place the thermometer in your child’s armpit and then bring your child’s arm to their side so they are “pinching” the thermometer in their underarm.
Temperatures in the axilla are consistently lower than rectal temperatures (and can vary widely). Add a degree to the axillary temperature to estimate the true temperature.
This can be a quick and less invasive way to screen a temperature in a newborn (but remember a rectal thermometer should be used to double check).
It is also an alternative to an oral thermometer in a child under 5 years.
Ear and forehead: Ear thermometers are thought to be much more accurate than forehead thermometers (in fact, I don’t recommend forehead thermometers—they are a little too approximate!).
Ear thermometers are an excellent alternative if a child cannot tolerate an oral thermometer.
Ear thermometers are my favorite types of thermometers for children 3 months to 5 years old—they are quick and fairly accurate.
Ear temperatures are thought to be equivalent to rectal temperatures, so a fever is 100.4°F and above.
Apart from newborns, the exact number usually isn’t what matters most—it’s how your child looks and acts.
How the Brain Controls Body Temperature
The Hypothalamus
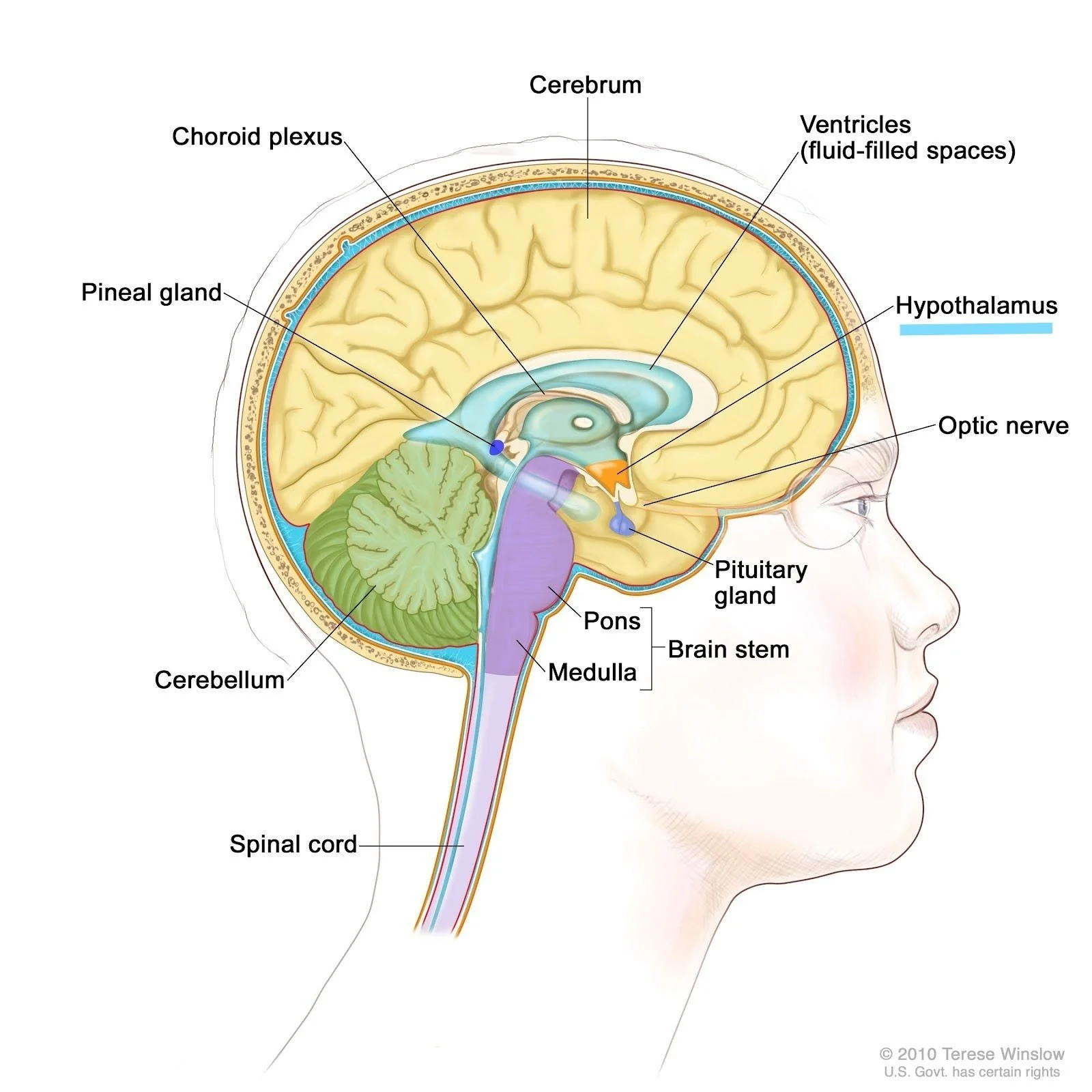
Deep in the brain sits the hypothalamus, your body’s thermostat. It’s almond-shaped, nestled right above the brainstem (the part that connects your brain to the spinal cord) and the pituitary gland (which releases hormones like growth hormone and thyroid-stimulating hormone), and below the thalamus (the relay center that directs most sensory and motor information).
The Thermoregulatory Center: Your Body’s Thermostat
Within the hypothalamus is the thermoregulatory center—the part of the brain that controls body temperature (Fun Fact: the hypothalamus also controls hunger and thirst). You can think of this as your body’s thermostat. It keeps temperature steady by balancing heat production (from metabolic activity in the muscles and liver) and heat loss (through sweating and fast breathing). If you’ve ever wondered why kids with fevers breathe fast and feel sweaty, this is why! Their bodies are using their intricate systems to try and cool off.
It is really pretty amazing, but our brains are able to maintain a fairly steady body temperature despite all the activity going on in our bodies. The only problem comes when we are exposed to very high environmental temperatures—above 95°F, the body’s ability to cool down is compromised and core body temperature can rise.
Fever vs. Hyperthermia
Our body temperature can rise from a fever or hyperthermia. We have been focusing on fever, but to understand why we don’t always get so nervous about a fever, it is important to know what distinguishes fever from hyperthermia.
And the key difference between fever and hypothermia comes down to the hypothalamic set point. A fever elevates your body’s hypothalamic set point, while hyperthermia does not. Let me explain:
Think of your child’s brain like a thermostat that controls body temperature. The hypothalamus decides what temperature the body should stay at—this is the set point.
If your child gets too cold, the body “turns on the heat” by shivering and conserving warmth. If they get too hot, the body “turns on the A/C” by sweating to cool down.
When your child has a fever, their brain temporarily raises the set point—like turning up the thermostat. That’s why they may shiver and feel cold at first, even though their temperature is rising. Despite the set point being higher than normal, the body is still able to keep things balanced and all body systems working as expected. Once the fever breaks, the thermostat resets and they sweat as their body cools back down.
In hyperthermia (like heat stroke) the hypothalamic set point is not reset, so it is like the thermostat is broken. The body can’t cool down even though it’s trying, which makes hyperthermia far more dangerous than a fever.
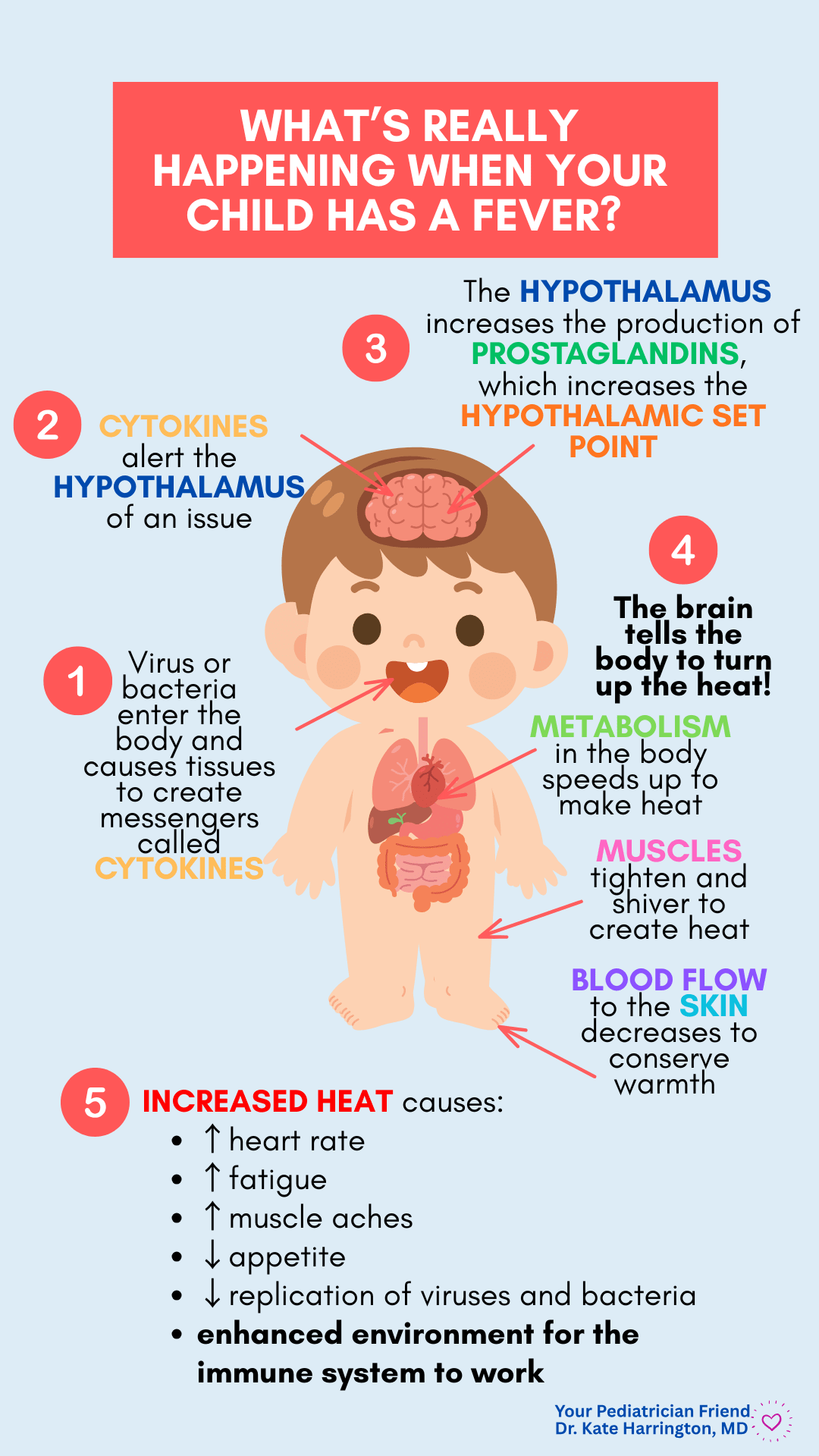
What’s Really Happening When Your Child has a Fever?
A fever isn’t just “getting hot”—it’s actually your child’s immune system hard at work.
Chemical Messengers Notify the Brain
When the body detects an infection, certain immune cells in your blood and tissue release special chemical messengers (called cytokines) that travel to the brain through the blood stream.
These messengers tell the hypothalamus (the body’s internal thermostat) to increase production of prostaglandins, which turn up the set point for temperature. In other words, the brain decides the body should be warmer to help fight off germs. And research suggests that bacteria and viruses are not able to grow as quickly at higher temperatures, and that immune system function is enhanced at higher temperatures.
The Brain Notifies the Body to Turn Up the Heat!
Once the hypothalamic set point is reset, the body works to raise its temperature to meet the new goal set by the hypothalamus:
Muscles tighten and shiver to create heat (what we call “the chills”),
blood flow to the skin decreases to conserve warmth,
and metabolism speeds up to generate more heat.
The body temperature rises until a new balance is achieved at the higher set point. The upper limit of temperature due to fever appears to be 42°C (107.6°F), but it is unusual for temperature to exceed 41°C (106°F).
Fever can also trigger other normal immune responses that are caused by cytokines—like faster heart rate, tiredness, achy muscles, and loss of appetite. These are all signs that the body is focusing its energy on fighting the source of the fever, and getting better.
Eventually, the Brain Tells the Body to Stand Down
When the immune system has been successful in fighting the infection, the cytokine messengers go away, the hypothalamic set point drops again, and the body cools down. This often manifests as sweating and flushed/red skin—what we often call “the fever breaking.”
So, while fevers can definitely be uncomfortable, they are usually a sign that your child’s immune system is doing exactly what it should! And, that’s a good thing!
When to be Concerned About a Fever
Most fevers are harmless—even the higher ones that make parents panic. But sometimes, fever can signal something more serious. The key is to pay attention to not just the number, but the whole picture: how your child looks, acts, and feels.
Here’s a simple rundown:
For babies under 2 months:
This is the big exception! If a baby under 2 months old has a rectal temperature of 100.4°F (38°C) or above, it is always considered an emergency.
Young infants do not have fully developed immune systems, and even a mild fever can be a sign of a serious infection.
Call your pediatrician or go to the emergency room immediately.
For babies over 2 months: fever is rarely dangerous. Call your pediatrician if your child:
Is 2-3 months old and has a temperature >100.4. As long as a child this age looks okay and is acting relatively normal, it is not an emergency. However, touch base with your doctor for any fever if your baby is under 3 months.
Has no symptoms of illness and the fever is lasting more than 3 days (72 hours)
Has symptoms of illness (like runny nose, cough, etc), and fever is lasting more than 5 days (120 hours)
Has a fever that goes over 104°F (40°C) and doesn’t come down with fever reducers
Looks very ill, unusually sleepy, or unresponsive
Has trouble breathing, persistent vomiting, or signs of dehydration (dry mouth, no tears, less than 1 wet diaper/pee every 8 hours)
Has a stiff neck, severe headache, or a rash that doesn’t fade (blanch) when pressed
Has a seizure
Has a chronic health condition or a weakened immune system that puts them at risk for more serious infections
Remember: fever is the body’s defense mechanism, not an enemy to be feared. It slows down viruses, boosts immune system activity, and helps the body to heal faster.
So while it is completely natural to want the number to go down, it’s okay to let your child’s immune system do its job—as long as they’re comfortable and staying hydrated.
How to Treat a Fever (and When You Don’t Have To!)
First, take a deep breath! You don’t need to spring into action every time the thermometer hits 100.4°F. A fever isn’t the body breaking down. It’s the immune system doing what it is designed to do! The goal isn’t always to make the fever go away, but instead to keep your child comfortable while their body does the hard work.
Focus on Comfort, Not the Number
If your child is playful, smiley (even just a little bit!), and hydrated, you don’t need to treat the fever. Really. Some kids can be 102°F and still be playing hard, while other kids are truly miserable at 100.8°F. Treat the child, not the temperature!
Hydration is Key
Fever makes the body lose fluids faster through sweating, faster breathing, and lower appetite. Offer frequent fluids: water, popsicles, soup, electrolyte drinks, or even jell-o if they will take it! Don’t worry about overall nutritional value—you are just concerned about getting them liquids.
Keep it Cool, but Not Too Cool!
Dress your child in lightweight clothes and use a light blanket if they are chilly. It might feel counterintuitive since they are burning up! But, their body will continue to think they are cold and keep raising their temperature. However, avoid bundling them up like they are stepping outside into a blizzard, as heavy blankets trap heat and will make them feel uncomfortable.
A lukewarm bath can help a child feel better, but skip cold baths or alcohol rubs. These just make them more uncomfortable and don’t help.
Medication: When to Use It
If your child is uncomfortable, has pain, or is having trouble sleeping, that’s when fever-reducing medication can help!
Acetaminophen (Tylenol) can be used in children over 2 months, and can be given every 4 hours.
Ibuprofen (Motrin or Advil) can be used in children over 6 months, and can be given every 6 hours.
Always consult a dosing chart and use your child’s weight, not their age, to determine the right amount. Check out my dosing chart here!
It can take up to 60 minutes for the medication to work. If your child is no better after 60 minutes, you can offer an alternative medication. Acetaminophen and ibuprofen are 2 different drugs, so there is no minimum time interval recommended between giving them. However, it is important to remember that acetaminophen can be given every 4 hours, and ibuprofen every 6 hours.
What Not to Do
Don’t wake a sleeping child just to give fever medicine. Sleep is healing, so wait until they wake up on their own and seem uncomfortable.
Don’t panic if the number doesn’t drop all the way to normal. Fever reducers typically bring a fever down by 1-2 degrees, not to 98.6°F.
Don’t worry if the fever comes back when the medicine wears off—that is just the immune system still at work!
Bottom Line
Fever is a sign that your child’s immune system is doing its job. Your job is to keep them hydrated, comfortable, and cared for! Extra hugs and kisses are appreciated! And a little screen time never hurts too. And if you are ever unsure, please call your pediatrician and talk it through.
Fever Myths and Misconceptions
Fever might be one of the most misunderstood (and feared) parts of parenting. Few things make parents more anxious than seeing that thermometer climb. But much of what we’ve been taught about fever is…well, wrong (thanks, Grandma and the internet!).
So, now that we’ve covered the science, let’s talk through a few common myths so you can rest a bit easier the next time your child feels warm.
Myth #1: Fevers can cause brain damage
Truth: Nope—not from the kind of fever your child gets from a virus or infection. The body’s internal thermostat (remember the hypothalamus?) won’t let the fever go high enough to cause brain damage. Fevers from infections rarely exceed 105°F (40.5°C), and damage doesn’t occur unless the temperature is over 108°F (42°C)—which is extremely rare and is almost always due to hyperthermia (heat stroke), not illness.
Myth #2: You always have to bring the fever down
Truth: The goal is for your child to feel comfortable, not to hit a specific number on the thermometer. Fever-reducing medications, like acetaminophen and ibuprofen, can help your child feel better while the immune system is hard at work, but they don’t “cure” the fever.
Myth #3: You should always alternate acetaminophen and ibuprofen every few hours when your child has a fever
Truth: Most of the time, using one medication will do the trick. Alternating medication can be confusing and increase the chances of mistakenly giving your child too much. If your child is truly miserable and can’t wait until the next dose is due, it is okay to alternate the medication as long as you are sure that there are 4 hours between each dose of acetaminophen and 6 hours between each dose of ibuprofen. However, this shouldn’t be your default strategy!
Myth #4: The higher the fever, the worse the illness
Truth: A sky high number on the thermometer does not always mean a severe or serious infection. Some mild viruses can cause very high fevers, while some serious bacterial infections could cause low grade ones. And some kids are just fever kids—no matter the illness, they always seem to spike high fevers. The important thing to look at is how your child looks and acts. If your child is alert, drinking fluids, and has some energy between fevers, that is generally a reassuring sign!
Myth #5: Sweating means the fever is breaking, and you should bundle them up to “sweat it out.”
Truth: Sweating is how the body cools itself down. So, this can definitely mean that the fever is starting to go away. However, don’t try to speed the process along by bundling your child up like you are sending them out on a subzero day! You will just make them even more uncomfortable!! Lightweight clothing and blankets are all they need.
Myth #6: You should give cold baths or alcohol rubs when your child’s fever is high
Truth: Absolutely not. Cold baths make kids shiver, which will actually raise their body temperature. And alcohol rubs can be absorbed through the skin and inhaled—which is unsafe. Stick to a cool washcloth or a lukewarm bath, but only if it is comforting for your child.
Myth #7: A normal temperature means they are better
Truth: I wish I could say this is 100% true, but it is very common for fevers to wax and wane as the immune system is doing its job. And sometimes it just takes the immune system a few days to get rid of those germs. So, don’t be worried if the fever comes back once the medicine wears off—that is normal. However, if the fever is gone more than 24 hours and then comes back, check in with your doctor to make sure something new isn’t brewing.
Myth #8: Teething causes high fevers
Truth: People talk about this all the time, but it is false. Teething might cause a slight temperature bump, but not fevers over 101°F. So, if your baby is teething and has a high fever, most likely they picked up some unwelcome germs while they were soothing their sore gums by chewing their hands or the Target cart.
Final Thoughts
A fever can look dramatic, but most of the time, it’s simply the body’s natural response to infection—not an emergency. You don’t need to panic, chase the number, alternate medicines every few hours, or doom-scroll through worst-case scenarios.
Instead, focus on what really matters:
How your child looks and feels
Whether they’re staying hydrated
Whether they’re getting better day by day
And remember—you know your child best. When in doubt, call your pediatrician. We’d always rather you reach out and feel reassured than stay up all night worrying.
Trust your instincts—you’ve got this!! 💕